Resilience Planning in Healthcare facilities post-COVID – 19
(Preparing for a future surge)
 Prof. Charanjit Singh Shah, Architect,
Prof. Charanjit Singh Shah, Architect,
Planner and Infrastructure expert, Art and Architecture critic
Founding Principal-Creative Group, Chairman-Smart Habitat Foundation, Senior Advisor-Assocham GEMS)
Introduction
Covid 19 has demonstrated that necessity is the mother of invention and has stretched many local, regional and national healthcare systems. When the very first case of coronavirus was recognised, we felt the need of isolation apartments and suddenly the demand of ventilators, mechanical systems started skyrocketing. A widespread stress was laid on the healthcare systems which brought variation in the sitting, eating and treatment arrangements. Globally the people were advised to stay safe at home which further gave rise to the economic crisis. This disease has led to a deep financial downturn for health care systems, as hospitals cancelled elective procedures and diagnostic services to reduce potential exposures and reallocate resources for expected COVID-19 patient surges.
It was clear by this time that our healthcare systems need to be redefined all-over particularly in this part of the subcontinent, where both private and public hospitals were not able to cope with the rising needs. It may be considered as an opportunity for us to redefine what we were lacking in.
Health care facilities form an important part of our society but are mostly seen in the light of functionality. With the changing times of post covid, we need to invoke a sense of a physically as well as physiologically healthy environment in hospitals and other healthcare facilities.
As well-said by Christine Nickl-Weller and Hans Nikal state: “sooner or later, all of us will enter a hospital: to give birth to a child, to visit a sick relative, to get treatment for an acute medical emergency, or indeed to say a farewell to a loved one.
Nature as a healer
Nature has always been closely associated with healing, as humans being an integral part of nature feel comfortable being in the domain of natural surroundings, but mostly it is seen that designers pay less attention to the ultimate aim of creating a healing environment. Various physical aspects of healing environment such as daylighting, mitigating the sense of isolation and disorientation are responsible in creating a sustained environment for healing. The building should offer an environment encouraging normalcy and allowing the person to recover.
Ar. Shamit Manchanda, Chairman, IIA Northern Chapter remarked in a webinar by Smart Habitat Foundation that as architects, resiliency in healthcare can be built first by creating a healing environment – connection with nature, natural light, soothing aesthetics, all psychologically help a person to heal. Functional considerations such as noise control and better acoustical performance, support systems and way finding are also imperative to create a resilient environment.
Since the advent of mankind, the importance of sunlight has been recognized and forgotten many a times. Ancient civilisations understood the critical importance of daylight associated with human health, happiness and wellbeing.  Access to natural light is one of the crucial aspects affecting the recovery of the patient. It influences the mood as well as the behaviour of the person. Daylight not only have the positive impact on patient’s outcomes, it also gives restorative benefits to other people in the surroundings.
Access to natural light is one of the crucial aspects affecting the recovery of the patient. It influences the mood as well as the behaviour of the person. Daylight not only have the positive impact on patient’s outcomes, it also gives restorative benefits to other people in the surroundings. 
The importance of the beneficial therapeutic effects of daylight and sunlight reached new levels of understanding with the treatment of tuberculosis (TB), rickets and jaundice becoming more widely understood in the early 1900’s.A new form of architecture was developed keeping the various benefits of sunlight in mind. Open spaces, huge windows welcomed the rays of sun filtering the darkness says Ar. Gurpreet Singh Shah, Principal Architect, and urbanist and infrastructure expert.
With the advent of air conditioning systems people started loving being indoors enjoying the crisp breeze of an air- conditioner. As a result, architecture and spaces also evolved accordingly. Similar to lymph nodes a direct contact with nature filters the toxic thoughts from a person’s mind and in today’s contemporary Architecture it has become necessity to start living as a robot in mechanical environment which has perhaps taken the human race away from nature.
Hospitals Before Covid
Hospitals these days are not less than a shopping mall, furnished with high technologies, waiting areas, cafeterias with a central air conditioning system abound. Hospitals are one of the largest and most complex of all modern institutions. They require a huge bureaucratic structure to run them. But slowly now, they have turned into robotic structures, working mechanically. Diagnosis and treatment are achieved by a scientific and machinery calculation managed by human wisdom but slowly and gradually human wisdom is reducing and our whole dependency is on machinery. There are piles of old jalopies and worn out bodies thrown at the back so as to present a welcoming look to the new clients. But patients are not machines, clinical and technical skills of those who treat patients are the highest priority. It seems like nothing human is left in humans, we are treated with machines, controlled by machines and now we have started living on machines.
Hospitals Post Covid
Epidemics have affected our environment, architecture as well as our living style. From interiors to city planning, our built environment is shaped by diseases. Previously, to minimize the risk of infectious diseases, people redesigned interior design, architecture, cities, and infrastructure. Considering historical events of the last two centuries, the architecture and urban story includes several developments.
 Dr Chandrasekhar, Former Chief Architect, Ministry of Health and Welfare, in a webinar of Smart Habitat Foundation highlighted the planning for a COVID operational hospital. He talked about the need for separation in the access points, bio containment unit, disinfection chamber, and various effective measures for maximum protection. In terms of material selection and cleanliness in the hospitals, he recommended switching to easy cleanable, non-porous, seamless, and microbial growth resistant materials. As for precautions and measures in building services and reduced air transmission of airborne diseases, negative pressurization in wards, toilets and corridors, and filtration and disinfection through air dilution and use of UV rays should be promoted.
Dr Chandrasekhar, Former Chief Architect, Ministry of Health and Welfare, in a webinar of Smart Habitat Foundation highlighted the planning for a COVID operational hospital. He talked about the need for separation in the access points, bio containment unit, disinfection chamber, and various effective measures for maximum protection. In terms of material selection and cleanliness in the hospitals, he recommended switching to easy cleanable, non-porous, seamless, and microbial growth resistant materials. As for precautions and measures in building services and reduced air transmission of airborne diseases, negative pressurization in wards, toilets and corridors, and filtration and disinfection through air dilution and use of UV rays should be promoted.
Changes In An Operation Hospital into Make-Shift Covid-19
Covid-19 has proved to be a milestone in the human history. With the overwhelming number of infected patients needing hospitalization, the need to expand the hospital facilities also need to enhance. Hence, the need of pre-fabricated materials, technologies and off-site construction came into being. Disinfection chambers have an entry point, an exit point, an enclosed chamber where the disinfection takes place, power supply, solvent supply, chemical chamber/mixer, air supply and compressor. Optional features include in chamber power outlets, lighting features, audio/video options, temperature scanners and chemical atomic.
Disinfection chambers have an entry point, an exit point, an enclosed chamber where the disinfection takes place, power supply, solvent supply, chemical chamber/mixer, air supply and compressor. Optional features include in chamber power outlets, lighting features, audio/video options, temperature scanners and chemical atomic.
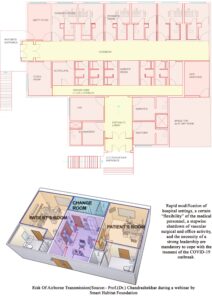
Rapid modification of hospital settings, a certain “flexibility” of the medical personnel, a stepwise shutdown of vascular surgical and office activity, and the necessity of a strong leadership are mandatory to cope with the tsunami of the COVID-19 outbreak. Rapid modification of hospital settings, a certain “flexibility” of the medical personnel, a stepwise shutdown of vascular surgical and office activity, and the necessity of a strong leadership are mandatory to cope with the tsunami of the COVID-19 outbreak.
 Holistic Approach
Holistic Approach
Sustainability is the most trending approach in the building industry so as to minimise the ecological footprint of the overall built up environment. From a building life cycle cost perspective, sustainable buildings are cheaper in the long run despite the somewhat higher capital investment. Hospitals are the second higher energy consumers on the per square foot basis after the food services. Moreover, hospitals have a special responsibility to ensure that their operations do not pose environmental harm.
Natural Ventilation
Before the introduction of mechanical ventilation in hospitals, natural ventilation was the primary mode of ventilation used in hospitals. In recent times, natural ventilation has been largely replaced by mechanical ventilation systems in developed and developing countries. With the rising interest in sustainability, natural ventilation has been ‘revived’ as a strategy to reduce building energy costs. Various design features influence the intake of natural ventilation: –
Orientation of the rooms: – To solve the apparent conflict between the best orientation from the solar aspect (south-north) and that optimal for ventilation, suitable design details such as orientating the windows at oblique angles to non-east facing walls to maintain effective ventilation or equipping east-facing windows with appropriate shading (architectural elements or vegetation) can be employed.
Size and detail of openings: – The location, number and size of openings determine the ventilation conditions of the building. The best window opening arrangement to maintain cross-ventilation in hot-humid climates is full wall openings on both the windward and leeward sides of the building. When the wind direction is at a very small angle (nearly parallel) to the wall, as in the case of an elongated building facing north and south in a region with winds from southeast to northeast, it is possible to create effective cross ventilation in a given room by having at least two windows in the windward wall, each with a single “wing wall” or vertical projection. Wing walls are useful low-energy devices that can help capture wind using a ‘fin’ at the façade to channel wind into the building interiors to increase the internal airflow per hour and so create internal conditions similar to the effects of a ceiling fan. In each one of these windows the projection should be installed on alternative (left and right) sides. The windows should preferably be vertical (i.e., narrow and high). One window will be in a wind pressure zone, acting as inlet, and the other window will be in the suction zone, acting as outlet. Architectural elements projecting in front of the main wall, such as alcoves or bookcases, with windows in front and behind them, can be as effective in enhancing ventilation.
Shading of Openings: – Fixed shading for windows should help to block the low sunrays for eastern and western walls. Inclined overhangs are also useful for shading if horizontal narrow strips of windows are used. In single-story buildings it is possible to shade the walls and the windows by wide verandas, designed as roof extensions, or overhangs, above the walls. Such overhangs form, in effect, a covered outdoor open area, shaded and protected from the rain. Shading by vegetation can also be provided relatively easily to low-rise buildings in hot-humid climates. For walls: significantly increase the insulation of walls to counteract the solar gain or maintain, by repeated painting (due to fungal growth), a white colour of unshaded walls so that the sun will help in drying the walls and reducing the growth of fungi.
Case Study of SARI Treatment Centre
Coronaviruses (CoV) are a large family of viruses that cause illness ranging from the common cold to more severe diseases such as Middle East respiratory syndrome (MERS-CoV) and severe acute respiratory syndrome (SARS-CoV). Hospitals and healthcare centres need to adopt various protocols to prevent it spread.
Screening in new healthcare facilities
- A distance of 2 m between staff and patients is required.
- Double fencing or a Plexiglas barrier can be used for the separation.
- Natural ventilation and exhausted air dilution should be ensured.
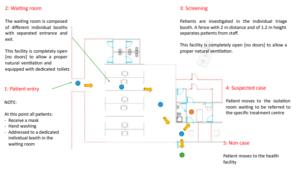
Waiting Room
The waiting room should be composed of individual booths open on both sides to ensure proper natural ventilation. Each booth should be clearly identified and labelled to avoid mistakes and allow patient flow. Booths should be cleaned and disinfected after each patient to avoid nose comial infections. If individual booths are not available, ensure a distance of at least 2 m between patients.
Screening Area (Source: -Severe Acute Respiratory Infections Treatment Centre, March 2020)
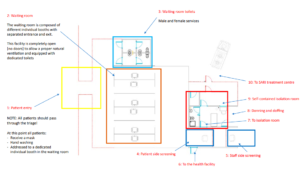 Minimum Requirements for converting a building into a Severe Acute Respiratory Infection Treatment Centre
Minimum Requirements for converting a building into a Severe Acute Respiratory Infection Treatment Centre
An existing building may be repurposed into a SARI treatment centre if the minimum requirements are met:
- minimum ventilation rate of 60 litres per second per patient for mild and moderate wards;
- minimum ventilation rate of 60 litres per second per patient for mild and moderate wards;
- airflow from clean to dirty zones;
- patient and staff flow can be clearly defined and distances respected;
- all finishes, furniture and patient care equipment can be effectively cleaned and are compatible with the facility’s disinfectants.
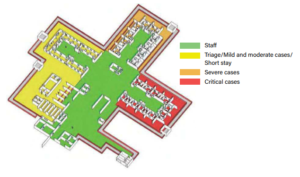
Severe Acute Infection Respiratory Treatment Centre Categorization
 Discharge Room
Discharge Room
This is for patients who do not fit the case definition or for mild and moderate cases referred to community facilities or homecare.
There should be a wide window on both sides to ensure adequate natural ventilation. Hand washing points must be available at the entrance and exit. A member of staff should always be present to control movements.
Conclusion
Coronaviruses are zoonotic, meaning they are transmitted between animals and people. Common signs of infection include respiratory symptoms, fever, cough, shortness of breath and breathing difficulties. With the increase in the number of cases globally, we need to take some immediate measures to control the spread by incorporating resilience techniques of planning as hospitals and health-care facilities play a critical role in this kind of situation. A direct connection with nature could help establishing a healing environment.